Artificial intelligence (AI) is no longer a futuristic concept in medicine—it is actively shaping how diseases are diagnosed, treated, and prevented. From analyzing medical images in seconds to predicting disease outbreaks and optimizing hospital workflows, AI is redefining healthcare delivery across the globe.
Healthcare systems face rising costs, aging populations, workforce shortages, and increasing chronic disease burdens. According to the World Health Organization, health systems must innovate to meet these challenges sustainably. AI offers a powerful toolkit: machine learning algorithms, natural language processing, robotics, and predictive analytics that enhance clinical decision-making and streamline operations.
This article explores how artificial intelligence is used in healthcare, covering real-world applications, benefits, challenges, ethical considerations, and future trends—grounded in credible research and authoritative insights.
What Is Artificial Intelligence in Healthcare?
Artificial intelligence in healthcare refers to computer systems capable of performing tasks that typically require human intelligence. These tasks include recognizing patterns, interpreting complex data, learning from experience, and making predictions.
The National Institutes of Health describes AI as a transformative force in biomedical research and clinical care. At its core, AI in healthcare relies on:
- Machine Learning (ML): Algorithms that learn from data to improve predictions
- Deep Learning: Advanced neural networks often used in imaging and diagnostics
- Natural Language Processing (NLP): Understanding and analyzing human language in medical records
- Computer Vision: Interpreting medical images
- Robotics and Automation: Supporting surgery and hospital logistics
These technologies are embedded in tools that assist clinicians rather than replace them.
AI in Medical Imaging and Diagnostics

Medical imaging is one of the most advanced areas of AI adoption. Radiology generates vast volumes of images daily—X-rays, CT scans, MRIs, ultrasounds—requiring careful interpretation. AI algorithms can analyze these images rapidly and flag abnormalities.
Research published in journals supported by the National Library of Medicine shows that deep learning models can detect conditions such as lung nodules, breast cancer, and diabetic retinopathy with high accuracy. In some cases, AI performs comparably to experienced radiologists when used as a decision-support tool.
Key Applications:
- Early cancer detection
- Stroke identification in emergency settings
- Fracture detection in X-rays
- Retinal disease screening
The U.S. Food and Drug Administration has approved numerous AI-based medical imaging devices, reflecting growing regulatory oversight and validation.
AI does not eliminate the radiologist’s role. Instead, it enhances efficiency by prioritizing urgent cases and reducing diagnostic errors.
AI in Predictive Analytics and Early Disease Detection
Healthcare generates massive data from electronic health records (EHRs), lab results, wearable devices, and genetic sequencing. AI systems can analyze these datasets to predict disease risk before symptoms appear.
The Centers for Disease Control and Prevention highlights how predictive analytics can improve public health surveillance. AI models help identify patterns in chronic diseases such as diabetes, heart disease, and hypertension.
Examples of Predictive AI in Action:
- Identifying patients at risk of hospital readmission
- Predicting sepsis hours before clinical deterioration
- Estimating cardiovascular risk using patient history and biomarkers
- Forecasting infectious disease outbreaks
Hospitals use AI-powered dashboards to intervene early—adjusting medications, recommending lifestyle changes, or scheduling preventive screenings.
AI in Drug Discovery and Pharmaceutical Research

Drug development traditionally takes over a decade and billions of dollars. AI significantly accelerates this process by identifying promising compounds, simulating molecular interactions, and predicting toxicity.
According to insights shared by the National Institutes of Health, AI-driven drug discovery platforms analyze biological datasets far faster than conventional laboratory methods.
How AI Speeds Up Drug Development:
- Screening millions of chemical compounds digitally
- Predicting drug-target interactions
- Identifying repurposing opportunities for existing drugs
- Optimizing clinical trial design
During global health emergencies, AI-assisted research has shortened early discovery timelines and improved collaboration between pharmaceutical companies and research institutions.
AI in Personalized Medicine
Personalized medicine tailors treatment to an individual’s genetic profile, lifestyle, and environment. AI makes this possible by analyzing genomic data and identifying patterns across populations.
The National Human Genome Research Institute explains that AI helps interpret complex genetic sequences to determine which treatments may be most effective for specific patients.
Applications Include:
- Cancer treatment selection based on tumor genetics
- Pharmacogenomics (predicting drug response)
- Precision dosing
- Targeted therapies
Instead of applying one-size-fits-all protocols, clinicians can use AI insights to customize treatment strategies, improving outcomes and minimizing side effects.
AI in Robotic Surgery and Clinical Procedures
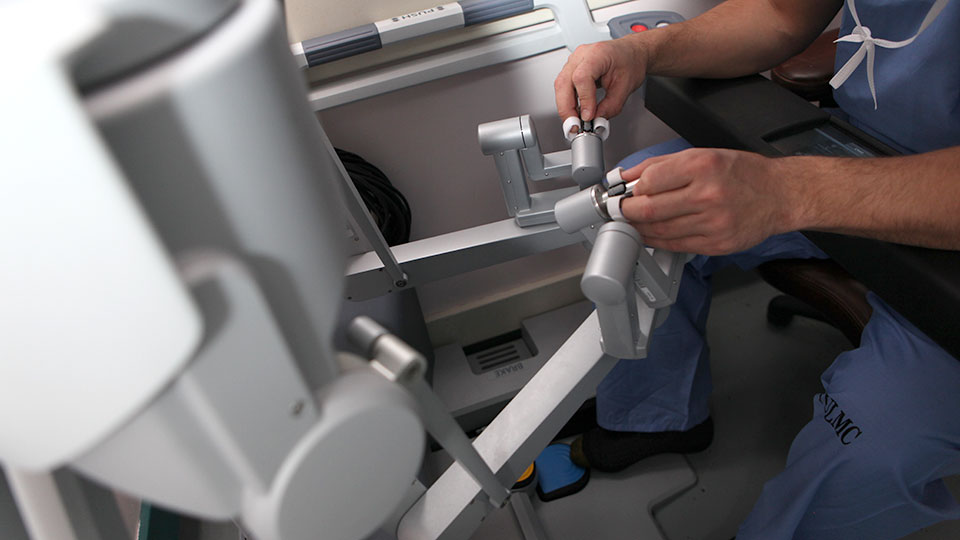
Robotic-assisted surgery combines AI algorithms with advanced mechanical systems to enhance precision. These systems translate a surgeon’s hand movements into smaller, more accurate actions.
Studies referenced by the Harvard Medical School indicate that robotic surgery can reduce complications, blood loss, and recovery time in certain procedures.
Benefits:
- Greater surgical precision
- Reduced invasiveness
- Shorter hospital stays
- Improved patient recovery outcomes
Importantly, AI does not perform surgery independently; trained surgeons remain fully in control.
AI-Powered Virtual Health Assistants and Chatbots
AI-driven chatbots and virtual assistants help patients schedule appointments, receive medication reminders, and access reliable health information.
The Mayo Clinic notes that digital health tools can enhance patient engagement and adherence to treatment plans.
Common Use Cases:
- Symptom triage guidance
- Chronic disease monitoring
- Mental health check-ins
- Remote patient support
These tools reduce administrative burdens on healthcare staff and provide round-the-clock assistance for patients.
AI in Hospital Administration and Workflow Optimization
Beyond clinical care, AI significantly improves operational efficiency.
Healthcare facilities manage complex logistics: staffing, bed allocation, billing, supply chain management, and appointment scheduling. AI algorithms analyze historical patterns to optimize these processes.
Operational Benefits:
- Reduced patient wait times
- Efficient staff scheduling
- Optimized inventory management
- Fraud detection in billing
The World Economic Forum highlights how AI-powered automation can lower operational costs while improving patient experience.
Comparison Table: Traditional Healthcare vs. AI-Enhanced Healthcare
| Feature | Traditional Approach | AI-Enhanced Approach |
|---|---|---|
| Diagnostic Speed | Manual image review | Automated image analysis within seconds |
| Disease Prediction | Reactive after symptoms | Predictive and preventive insights |
| Drug Discovery | Lab-based, time-intensive | Computational screening & modeling |
| Treatment Planning | General guidelines | Personalized, data-driven decisions |
| Administrative Tasks | Manual processing | Automated workflow optimization |
| Patient Monitoring | In-person visits | Remote monitoring & AI alerts |
AI augments clinical expertise, enabling faster and more data-informed decisions.
Ethical Considerations and Data Privacy
AI in healthcare raises important ethical questions. Patient data must be protected, and algorithms must be transparent and unbiased.
The World Health Organization emphasizes responsible AI governance, including fairness, accountability, and transparency.
Key Ethical Concerns:
- Data privacy and cybersecurity
- Algorithmic bias
- Informed consent
- Regulatory oversight
Healthcare providers must ensure AI tools comply with regulations and undergo rigorous validation before implementation.
Challenges Limiting AI Adoption
Despite its promise, AI adoption faces obstacles:
- Integration with existing hospital systems
- High implementation costs
- Limited high-quality training data
- Resistance to technological change
- Regulatory uncertainty
The U.S. Food and Drug Administration continues refining frameworks for AI-based medical devices to ensure safety and effectiveness.
Healthcare institutions must balance innovation with patient safety.
The Future of Artificial Intelligence in Healthcare
AI is expected to expand into new areas:
- Real-time wearable health analytics
- Advanced genomics integration
- AI-guided mental health support
- Remote robotic procedures
- Global disease surveillance networks
As computing power increases and datasets grow, AI systems will become more accurate and adaptive.
The long-term vision is collaborative intelligence—where human clinicians and AI systems work together to deliver better care.
Frequently Asked Questions (FAQ)
1. Is artificial intelligence replacing doctors?
No. AI serves as a decision-support tool. Clinicians remain responsible for final diagnoses and treatment decisions.
2. How accurate is AI in diagnosing diseases?
Accuracy varies by application. In imaging and pattern recognition tasks, AI has shown performance comparable to specialists when validated in clinical settings.
3. Is patient data safe when using AI?
Healthcare organizations must comply with strict data protection laws and cybersecurity standards to safeguard patient information.
4. Can AI reduce healthcare costs?
Yes. AI improves efficiency, reduces diagnostic errors, optimizes resource use, and accelerates drug discovery, potentially lowering overall costs.
5. What are the risks of AI in healthcare?
Risks include biased algorithms, data breaches, and overreliance on automation. Proper oversight and regulation are essential.
Conclusion: A Smarter, Safer, More Predictive Healthcare System
Artificial intelligence is reshaping healthcare at every level—from diagnostics and drug discovery to surgery and hospital management. By analyzing vast datasets quickly and accurately, AI enables earlier disease detection, personalized treatments, and more efficient operations.
However, successful integration requires responsible governance, rigorous validation, and continuous human oversight. Ethical considerations, data security, and regulatory compliance must remain central to AI deployment.
The healthcare landscape is evolving toward predictive, preventive, and precision-based care. AI acts as an enabler, strengthening—not replacing—the expertise of medical professionals.
As global health challenges grow more complex, the collaboration between clinicians, researchers, technologists, and policymakers will determine how effectively AI improves patient outcomes. The future of medicine lies in intelligent systems working alongside compassionate healthcare providers to deliver safer, smarter, and more accessible care worldwide.
